PICTURE THIS: you’ve been injured at work, and the last thing you want to do is answer a bunch of questions from a stranger or complete burdensome paperwork. You are likely in pain and feeling uncertain about your future, and now, in order to secure needed benefits, you’re expected to navigate the often-confusing workers’ compensation system…
While this is a generalization of what injured workers may experience, the evidence is more than anecdotal. According to recent industry data, U.S. adults have critical knowledge gaps about workers’ compensation. What’s more, Healthesystems’ own annual industry survey consistently shows that unfamiliarity with the workers’ comp system is one of the biggest barriers to injured worker recovery.
Let’s look at what people get wrong about workers’ comp – and how we can use meaningful engagement to help injured workers navigate this complex process.
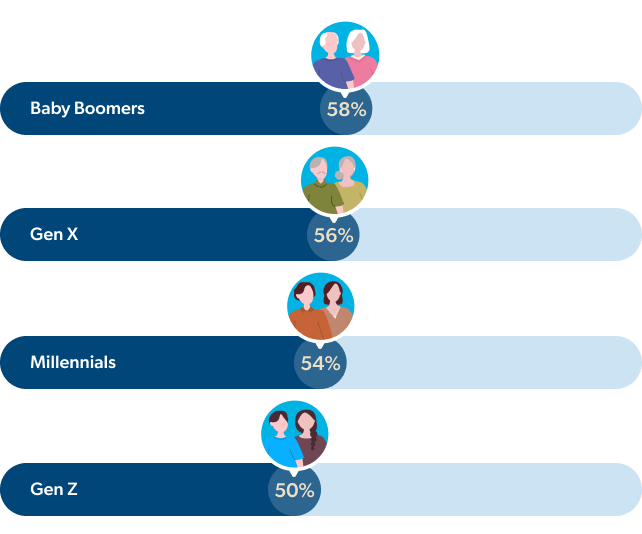
A 2025 survey of 1,000 U.S. adults shows that people have widespread misconceptions about workers’ comp in many areas, including basic rules and legal protections. For instance, fewer than 60% of respondents in any age group/generation correctly answered questions about eligibility and benefits – and this knowledge gap is actually more prevalent in the younger generations. Even more surprising, only 29% of respondents correctly understood that insurance companies (not employers) pay workers’ comp benefits.1
Other misconceptions revealed in the study include:
And while the majority of respondents (54%) described their experience with the workers’ compensation system as positive, many still considered filing for workers’ compensation difficult – with paperwork being the most difficult part.2
Lack of knowledge about workers’ compensation doesn’t just making filing for workers’ comp difficult – it can become an impediment to recovery. In Healthesystems’ 2026 survey of over 500 workers’ comp stakeholders, just over half of respondents (51%) ranked injured worker disengagement/unfamiliarity with the workers’ comp system as the biggest barrier to recovery. And among healthcare providers specifically, unfamiliarity ranked as the number one barrier (ahead of comorbidities/poor worker health) in both the 2026 and 2025 surveys.5
In a different study completed in 2021, Healthesystems found that half of injured workers delayed reporting their injuries due to the complexity of the workers’ comp system and lack of clarity. Difficulty navigating the system is also frequently cited, at least anecdotally, as one of the reasons injured workers hire workers’ comp attorneys.6
Unfamiliarity with the workers’ comp system doesn’t end with injured workers; it can extend to retail pharmacists, employers, even healthcare providers. For instance, a study based on interviews with administrators and providers from eight Community Health Centers (CHCs) in Massachusetts showed that lack of familiarity with the workers’ comp system actually discouraged their CHC’s use of workers’ comp for patient care.8
This begs the question: If physicians don’t even understand the system, who is there to help guide the injured worker? The answer lies in the claims team. In workers’ comp, the claims team is there for every part of an injured worker’s recovery journey. They handle the end-to-end process of managing claims, including communicating directly with injured workers, gathering supporting documentation, coordinating medical treatment, and facilitating return to work.
This gives claims teams a perfect opportunity to focus on the human aspects of patient engagement – essentially guiding injured workers through the process. Doing this well requires not just empathy and expertise, but systems and tools that support claims professionals in their day‑to‑day work rather than slowing them down.
To be truly engaged, injured workers need the right information, right at their fingertips. That’s why it’s important that claims teams are equipped with technology that makes their jobs easier and more efficient – removing administrative friction so they can focus on what matters most: supporting injured workers through the recovery process.
This includes digital engagement capabilities such as text messaging, mobile apps, and electronic document exchange, but also broader tools that streamline workflows, simplify documentation, and reduce unnecessary back‑and‑forth.
To dive deeper into digital engagement, read the article in this issue titled “Influential Engagement: How Purposeful Digital Strategies Drive Positive Patient Participation.”
In addition to claims teams, partners with deep expertise in workers’ compensation processes can play a useful supporting role in the injured worker’s journey. Depending on where they engage in the system, these partners can help reinforce education, reduce friction, and provide guidance at key moments – complementing the efforts of claims professionals, employers, and healthcare providers.
For example, Pharmacy Benefit Managers (PBMs) can perform collaborative outreach and intervention at multiple touchpoints across the care continuum – with injured worker patients, pharmacists, and prescribers – to positively impact outcomes. Examples of this support may include:
By deploying workers’ comp experts at impactful touchpoints in the injured worker’s journey, we can supplement the guidance they may receive from their employer and physician to support smoother workers’ comp experiences and, ideally, better health outcomes.
