Industry stakeholders in all areas of workers’ comp – from employers to insurance brokers, claims adjusters to executive leaders – are concerned about increasing claims complexity with over 65% citing it as a top challenge in our recent survey.1 Although the overall number of claims continues to decrease nationwide, more routine claims are escalating and taking longer to close at higher costs. According to the National Council on Compensation Insurance (NCCI), from 2014 – 2018 lost-time claim severity increased by 3.4% and medical claim severity increased by 2.9%.2
The reasons that claims are becoming more difficult to process and conclude are somewhat complicated in themselves. Poor worker health and chronic conditions, such as obesity, hypertension, and diabetes, along with psychosocial factors, such as anxiety and depression, troubled home life, and inability to cope with the challenges of an injury, can significantly affect an injured worker’s recovery. And the impact of comorbidities has been well documented, including findings that claims with comorbidities have medical costs that are double those of similar claims without a comorbidity diagnosis.3
Comorbidities and psychosocial issues are not new, of course, but they are more prevalent in workers’ comp, largely due to the changing workforce population. The U.S. workforce is getting older. By 2024, nearly 25% of workers will be over 55,4 accounting for the largest segment of the workforce, and approximately 80% of those are likely to have at least one chronic condition.5 At the same time, millennials (aged 23-38) currently make up the largest segment of the workforce and they are more likely to experience anxiety and depression.6 Add to those demographic shifts the combination of widespread legislation mandating coverage for mental health exposures, a range of social and economic ills, from the opioid crisis to inadequate group health insurance, and changing medical trends, including a shift to other potentially risky drugs for pain relief, such as NSAIDs and anticonvulsants, and the result is a higher percentage of complex claims.
The consequences of this trend are serious and it is a top concern for industry stakeholders, as indicated by its ranking as the #1 challenge for workers’ comp programs in 2020.1 Payers face higher indemnity and medical costs, injured workers suffer delayed recoveries and suboptimal outcomes, and claims and care professionals, whose numbers are also decreasing due to retirements, have to manage larger and more difficult caseloads.
Complex claims are a complex problem and there is no single solution. But there are some tools and best practices to help manage these claims as efficiently and effectively as possible and, ideally, reduce their numbers.
When it comes to managing medical care, early decisions are crucial. Most claims are not complex from the beginning. They start out with a typical injury and become complex over time through a series of seemingly small decisions and routine actions that can quickly add up. The most important step in avoiding claim escalation is to recognize and flag those claims that pose risks.
Of course, there are many more potential risks and the task of identifying each and every one would be daunting, even for the most experienced claims professionals. This is an area where technology can do much of the legwork. Data analytics can be used to identify patterns over time and apply that intelligence to individual risk indicators as they arise. Claims and benefit management systems may provide risk scores and other reports to call out claims that merit review, monitoring, and intervention. Ensuring that you have a robust solution that integrates information from across the continuum of care is essential to identifying risks early and accurately.
"MUCH OF THE IMPORTANT INFORMATION IN THE PATIENT RECORD DOES NOT EXIST AS DISCRETE DATA POINTS."
As technology continues to advance, these capabilities are becoming even stronger. Currently, much of the most important information in the patient record does not exist as discrete data points, but only as text, often in the form of notes. With artificial intelligence (AI) and machine learning tools, such as natural language processing (NLP), crucial details from patient records in various systems, such as medical notes from physicians, physical therapists, pharmacists, and home health aides, can be extracted and stored as data elements that drive analytics methodologies to provide actionable information. The data modeling becomes more accurate with greater amounts of data, so predictive capabilities will increase with more records and over greater periods of time.
Once at-risk claims are identified, they can be routed to the correct experts, such as nurse case managers or clinical pharmacists, and assessed for immediate intervention or monitoring, as appropriate. The key to avoiding unnecessary escalation is to channel these claims along a path for extra scrutiny as soon as a risk warning is identified. This makes it easier for claims professionals to give their attention where it is most needed, while allowing the low-risk claims to continue along a more typical and automated path.
The siloed nature of our healthcare system can make care management difficult. Patients who have multiple health concerns receive care from different medical providers and may need a variety of treatment modalities. Keeping track of physicians, prescriptions, equipment, and medical services, such as physical therapy and home health aide, is challenging and cannot be met with human resources alone.
Claims processing software has long been useful for keeping records and completing administrative tasks. Many of the growing number of clinical decisions that claims professionals must now make can be automated, thanks to embedded evidence-based guidelines, drug formularies, utilization review rules, etc. But a comprehensive view of patient care is key to efficient claims management and avoiding complications. Not to mention that predictive data can only be captured and utilized if it can be accessed. For these reasons, maximum technical integration with providers and partners should be a priority in reducing unnecessary claims escalation.
Various interventions are often required to keep a claim from going off course, or to get it back on the right path. Common clinical interventions include provider outreach to request additional information about treatment, express concerns, or provide education regarding evidence-based guidelines, formularies, therapeutic alerts, etc. Providers are often unaware that their patients are being treated by other physicians or therapists and even that they are taking multiple medications, so communication and care coordination is essential for optimal patient recovery.
Direct engagement with patients can also help keep claims on a good trajectory. Studies have shown that patient engagement is effective at reducing medical costs and improving health outcomes (see Patient Engagement is Personal: How to Help Injured Workers Help Themselves, RxInformer Winter 2018-19). Patient engagement can include various initiatives, including patient portals and mobile apps, medication therapy management programs, psychosocial evaluations, wellness education, and medication adherence.
Both prescriber intervention and patient engagement can require additional time and money, but good programs should more than pay for themselves by reducing claims complications and costs.
The changing population, generally poorer worker health, and expanding coverage for non-traditional injuries and conditions make more complex claims inevitable. The average medical cost on lost-time claims has more than tripled over the last 20 years and is now approximately $30k, an increase that has outpaced medical price inflation by 146%.7 This trend is largely due to the demand for more medical services. So, it is important to explore new ways to deliver those services as cost-effectively as possible.
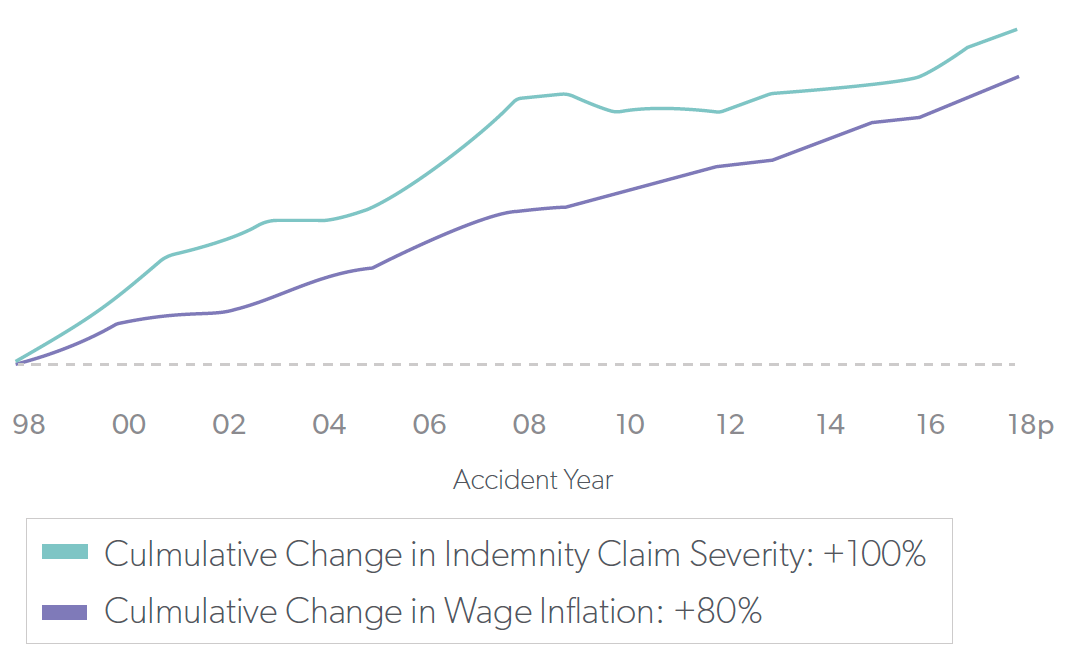
Source: NCCI8
Again, some of the most promising solutions are likely to come from technology. Telemedicine has the potential to help injured workers receive treatment more quickly and affordably, and the use of remote medical monitoring devices are an excellent way to manage chronic conditions. Telerehabilitation is proving effective with one recent study showing that it produces similar results to in-clinic rehabilitation.9 And the rapidly growing field of digital therapeutics is showing great promise, particularly in the area of cognitive behavioral therapy (CBT), which could be a great help in treating patients with psychosocial conditions.
Good technology is an invaluable tool in managing – and minimizing – complex claims in workers’ compensation. But technology does not replace human judgment, clinical expertise, and care. On the contrary, its ultimate benefit is expanding the capacity of claims and care managers to focus their attention on the patients who need it most. When surveyed, 82% of workers’ comp professionals agreed that improved claims efficiency could reduce medical costs.1 And that’s because a streamlined claims management process, with people and technology working together, can get the right care for the right patients at the right time.
